Thomas Maouris, Peter Del Mar, Nathan Brown, Lachlan Abbot, Mathilda Thorrowgood
ABSTRACT 
Objective
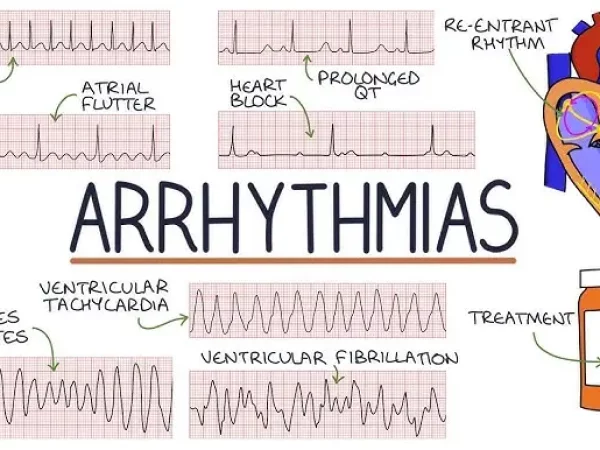
To assess adherence to international anticoagulation guidelines in emergency department (ED) patients undergoing direct current cardioversion (DCCV) for atrial fibrillation (AF) or flutter, and to describe associated outcomes.
Methods
A retrospective study was conducted at a metropolitan ED (January 2020–December 2023). Of 410 AF/flutter presentations, 158 patients (mean age 57 years; 83.5% male) underwent DCCV. Data on arrhythmia characteristics, anticoagulation timing, and outcomes were reviewed using 2024 European Society of Cardiology criteria.
Results
AF was present in 91.1% and flutter in 8.9% of cases. Most arrhythmias were recent onset (71.5% < 24 h; 10.1% < 48 h), with no precipitant identified in 87.3%. Rivaroxaban (48.7%) and apixaban (22.1%) were the most prescribed anticoagulants. After cardioversion, 76.6% of patients were discharged directly from ED, 12.7% transferred to short-stay, and 10.1% admitted. Adherence to anticoagulation guidelines was achieved in 94% of cases pre-cardioversion and 90% post-cardioversion, with appropriate DOAC dosing in 88.2%. Patients with CHA2DS2-VA ≥ 2 were significantly more likely to receive appropriate therapy (p < 0.01). ED revisit rates were 17.1% at 30 days and 46.2% at 12 months, often related to recurrent AF.
Conclusion
Most patients undergoing ED cardioversion received guideline-concordant anticoagulation. However, variability in dosing and post-procedural therapy persists, particularly among low-risk patients. High revisit rates highlight the need for improved follow-up, continuity of anticoagulation, and structured care pathways following ED cardioversion.