Written by Denrick Cooper
Spoon Feed
Postpartum hemorrhage (PPH) is a high-risk, low-frequency ED emergency. This review provides a practical, ED-focused approach centered on the “4 Ts”—Tone, Tissue, Trauma, and Thrombin—with clear guidance on early recognition and rapid escalation.
Know the 4 Ts
We’ve covered this before, but it’s time for a refresh. PPH remains a leading cause of maternal morbidity and mortality worldwide. Patients may present after discharge or following a precipitous delivery, and early recognition is tricky because vital signs can look deceptively normal despite significant blood loss. PPH is defined as ≥1000 mL blood loss within 24 hours of delivery or any bleeding associated with hypovolemia and can occur up to 12 weeks postpartum.
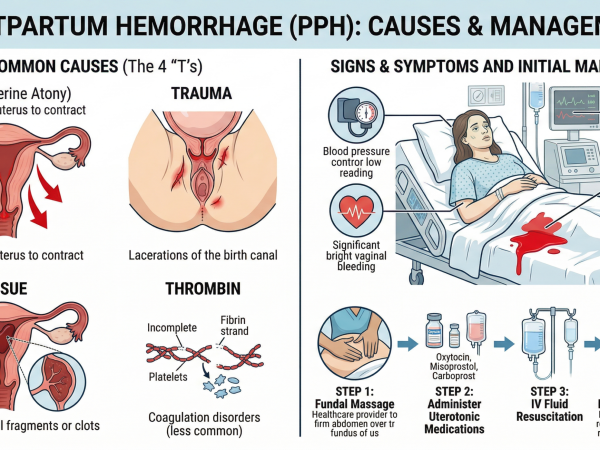
Causes—the “4 Ts”: Tone, Tissue, Trauma, and Thrombin.
Uterine atony (Tone) is by far the most common, so it should be assumed first. A boggy, enlarged uterus points toward atony, while a firm uterus with continued bleeding should shift your thinking toward trauma (Trauma), retained tissue or clot (Tissue), or coagulopathy (Thrombin). In reality, patients often have more than one cause.
Management should be immediate and parallel:
- Rapid hemodynamic assessment, large-bore IV, labs (CBC, coags, fibrinogen, and type and cross) and pelvic exam
- Uterine massage/compression
- Empty the bladder
- Oxytocin first-line
- Add second-line uterotonics (methylergonovine, carboprost, misoprostol)
- Give TXA 1 g IV early (within 3 hours), with repeat dosing if needed.
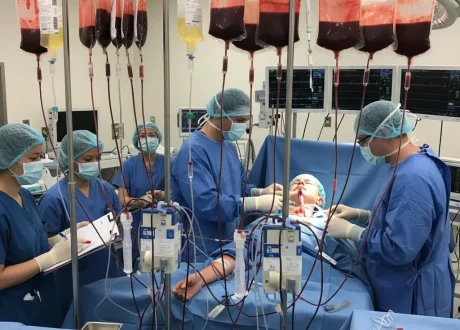
- Have a low threshold for blood products and massive transfusion, with attention to fibrinogen.
- If bleeding persists, escalate quickly to balloon tamponade or IR embolization or surgery.
Address the cause: repair lacerations, remove retained products, correct coagulopathy, and recognize rare but critical diagnoses such as uterine inversion or rupture.
How does this change my practice?
This was a good reminder of how high risk PPH really is, and how easy it is to miss early. The 4 Ts give me a simple way to stay organized in real time. I’ll have a lower threshold to act early and escalate quickly, rather than waiting for obvious instability. It also reinforces the importance of calling OB early and using the full team. Having a quick, accessible ED reference (something like a pocket guide) may also be helpful in these high-stress, time-sensitive, low-frequency situations.
Source
High risk and low incidence diseases: Postpartum hemorrhage. Am J Emerg Med. 2026 May;103:65-72. doi: 10.1016/j.ajem.2026.01.048. Epub 2026 Jan 29. PMID: 41653849.
Written by Denrick Cooper
Spoon Feed
Postpartum hemorrhage (PPH) is a high-risk, low-frequency ED emergency. This review provides a practical, ED-focused approach centered on the “4 Ts”—Tone, Tissue, Trauma, and Thrombin—with clear guidance on early recognition and rapid escalation.
Know the 4 Ts
We’ve covered this before, but it’s time for a refresh. PPH remains a leading cause of maternal morbidity and mortality worldwide. Patients may present after discharge or following a precipitous delivery, and early recognition is tricky because vital signs can look deceptively normal despite significant blood loss. PPH is defined as ≥1000 mL blood loss within 24 hours of delivery or any bleeding associated with hypovolemia and can occur up to 12 weeks postpartum.
Causes—the “4 Ts”: Tone, Tissue, Trauma, and Thrombin.
Uterine atony (Tone) is by far the most common, so it should be assumed first. A boggy, enlarged uterus points toward atony, while a firm uterus with continued bleeding should shift your thinking toward trauma (Trauma), retained tissue or clot (Tissue), or coagulopathy (Thrombin). In reality, patients often have more than one cause.
Management should be immediate and parallel:
- Rapid hemodynamic assessment, large-bore IV, labs (CBC, coags, fibrinogen, and type and cross) and pelvic exam
- Uterine massage/compression
- Empty the bladder
- Oxytocin first-line
- Add second-line uterotonics (methylergonovine, carboprost, misoprostol)
- Give TXA 1 g IV early (within 3 hours), with repeat dosing if needed.
- Have a low threshold for blood products and massive transfusion, with attention to fibrinogen.
- If bleeding persists, escalate quickly to balloon tamponade or IR embolization or surgery.
Address the cause: repair lacerations, remove retained products, correct coagulopathy, and recognize rare but critical diagnoses such as uterine inversion or rupture.
How does this change my practice?
This was a good reminder of how high risk PPH really is, and how easy it is to miss early. The 4 Ts give me a simple way to stay organized in real time. I’ll have a lower threshold to act early and escalate quickly, rather than waiting for obvious instability. It also reinforces the importance of calling OB early and using the full team. Having a quick, accessible ED reference (something like a pocket guide) may also be helpful in these high-stress, time-sensitive, low-frequency situations.
Source
High risk and low incidence diseases: Postpartum hemorrhage. Am J Emerg Med. 2026 May;103:65-72. doi: 10.1016/j.ajem.2026.01.048. Epub 2026 Jan 29. PMID: 41653849.
Postpartum hemorrhage (PPH) is a high-risk, low-frequency ED emergency. This review provides a practical, ED-focused approach centered on the “4 Ts”—Tone, Tissue, Trauma, and Thrombin—with clear guidance on early recognition and rapid escalation.
Know the 4 Ts
We’ve covered this before, but it’s time for a refresh. PPH remains a leading cause of maternal morbidity and mortality worldwide. Patients may present after discharge or following a precipitous delivery, and early recognition is tricky because vital signs can look deceptively normal despite significant blood loss. PPH is defined as ≥1000 mL blood loss within 24 hours of delivery or any bleeding associated with hypovolemia and can occur up to 12 weeks postpartum.
Causes—the “4 Ts”: Tone, Tissue, Trauma, and Thrombin.
Uterine atony (Tone) is by far the most common, so it should be assumed first. A boggy, enlarged uterus points toward atony, while a firm uterus with continued bleeding should shift your thinking toward trauma (Trauma), retained tissue or clot (Tissue), or coagulopathy (Thrombin). In reality, patients often have more than one cause.
Management should be immediate and parallel:
- Rapid hemodynamic assessment, large-bore IV, labs (CBC, coags, fibrinogen, and type and cross) and pelvic exam
- Uterine massage/compression
- Empty the bladder
- Oxytocin first-line
- Add second-line uterotonics (methylergonovine, carboprost, misoprostol)
- Give TXA 1 g IV early (within 3 hours), with repeat dosing if needed.
- Have a low threshold for blood products and massive transfusion, with attention to fibrinogen.
- If bleeding persists, escalate quickly to balloon tamponade or IR embolization or surgery.
Address the cause: repair lacerations, remove retained products, correct coagulopathy, and recognize rare but critical diagnoses such as uterine inversion or rupture.
How does this change my practice?
This was a good reminder of how high risk PPH really is, and how easy it is to miss early. The 4 Ts give me a simple way to stay organized in real time. I’ll have a lower threshold to act early and escalate quickly, rather than waiting for obvious instability. It also reinforces the importance of calling OB early and using the full team. Having a quick, accessible ED reference (something like a pocket guide) may also be helpful in these high-stress, time-sensitive, low-frequency situations.
Source
High risk and low incidence diseases: Postpartum hemorrhage. Am J Emerg Med. 2026 May;103:65-72. doi: 10.1016/j.ajem.2026.01.048. Epub 2026 Jan 29. PMID: 41653849.