Spoon Feed
In patients with acute pulmonary embolism (PE), only supraventricular tachycardia (SVT) was an independent predictor of clinical deterioration (CD); however, other ECG findings (below) were associated with abnormal RV function (abnl-RV) on echo.
Why does this matter?
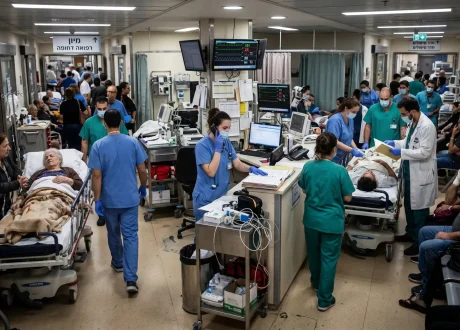
As emergency physicians, PE should always be on our differential for chest pain, shortness of breath, syncope, etc. Once we’ve found a PE, it is helpful to have a sense of who might need a higher level of care to prevent CD, particularly as these patients remain boarded in our departments. Having parameters by which we can risk-stratify patients gives us a sense of who needs a little more attention.
Take my breath away…
This was a prospective, multicenter study of 1,736 newly confirmed PE patients. Of the 1,629 patients with both ECG and echo, ~25% experienced CD, defined as respiratory failure, hypotension, dysrhythmia, cardiac arrest, escalated PE intervention, or death within 5 days. Of the same 1,629 patients, ~32% had abnl-RV, which had an OR for CD of 4.25 (3.35, 5.38). On the other hand, absence of abnormal ECG findings had an OR for CD of 0.34 and abnl-RV 0.24, both statistically significant.
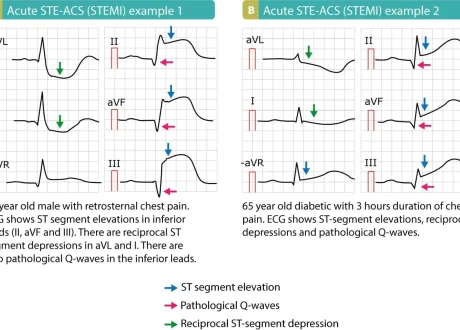
Only one ECG pattern had a significant OR of 2.87 for CD – SVT. T-wave inversions in V2-4, incomplete right bundle branch block, ST elevation in aVR, sinus tachycardia, and S1-Q3-T3 were all independent predictors of abnl-RV on echocardiogram.
Source
Electrocardiographic findings associated with early clinical deterioration in acute pulmonary embolism. Acad Emerg Med. 2022 Jun 24. doi: 10.1111/acem.14554. Online ahead of print.