**This week Dr. Josh Kessler and I tackle hypothermia and the complicated art of a hypothermic resuscitation. Dr. Kessler is a fellow of the academy of wilderness medicine and an excellent teacher. Thanks for your help, Josh!**
As you walk into your shift, you hear the staff buzzing around with more enthusiasm than normal for a 6 am shift. “Doc! Glad you’re here! They think they found him!” you hear one of the techs tell you.
“Wha… what’s going on?” you ask, coffee not quite kicking in yet.
“The missing snowboarder. A 19-year-old kid; went out on the mountain yesterday; never came back to the lodge afterwards. He’s an avid snowboarder, so family thought he was just doing extra runs. By the time they alerted mountain patrol, it was dark and snowing, almost impossible to find anything out there. They’ve been looking all night and hadn’t found him yet, but one of my buddies is on the rescue team and, rumor is, they think they may have found him!”
“This is mountain rescue team 1529 calling for stat medical command. Over.”
“I knew it, doc!” you hear the tech say. “We’ll go prep a room; you talk to the rescue team.”
“Go ahead rescue team 1529”
“Hey Doc, good news, we found the snowboarder! He’s been missing since yesterday, so he’s in rough shape. He’s unresponsive and extremely cold to the touch. We have a very weak pulse; getting him loaded up and should be down the mountain to you in about 15-20. Be ready for us. Rescue team 1529 out.”
You and the team hustle to get a room ready for the patient and get the rewarming equipment ready.
The rescue team arrives and the patient does not look well. “Hey, Doc, like we said, extremely cold to the touch, unresponsive. We wrapped him in blankets and came as quick as we could. Not a ton more history to give you. Good luck!”
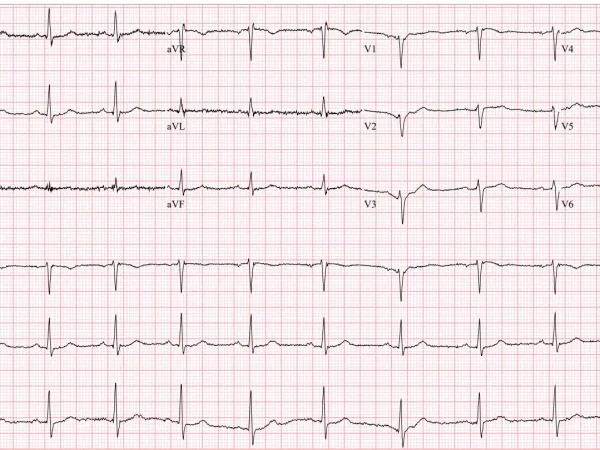
You and the team start working on the patient. He has an extremely weak pulse. Core temperature is 28℃ (82℉). As you and the team start setting up the rewarming process, you get a quick ECG:
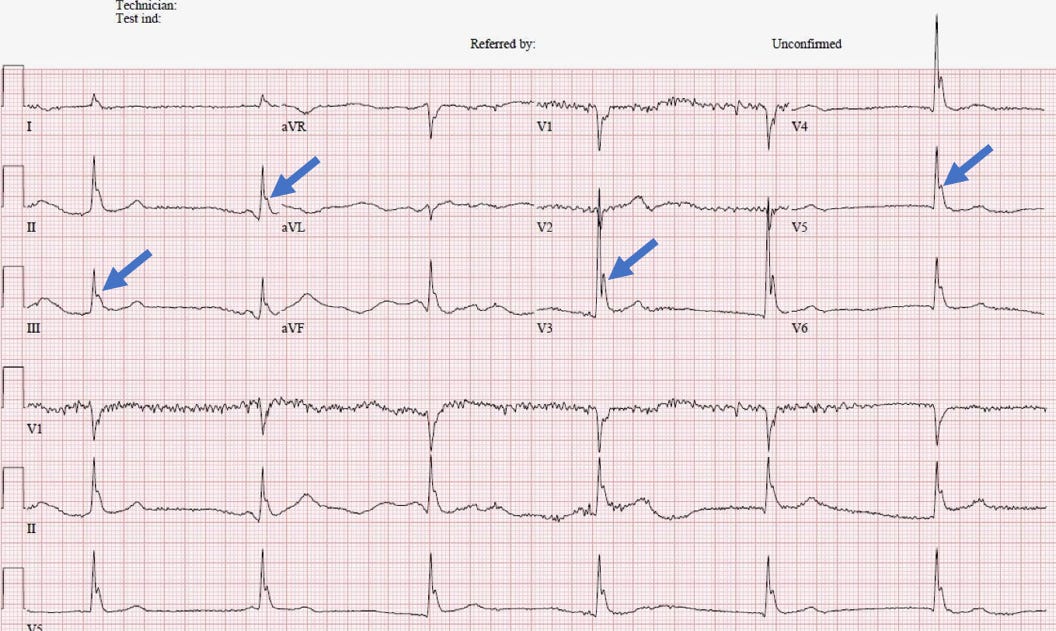
Rate: 36
Rhythm: A little bit hard to tell. Either sinus bradycardia or a junctional escape rhythm, but I’m leaning junctional escape rhythm. It could also be an AV block, since they’re common with severely hypothermic patients, but, pretty hard to find definitive P waves.
Axis: Normal
Intervals: Tough to see definitive P waves here given the significant artifact, QRS narrow, QTc is reasonable.
Morphology: Now the fun part. There’s an extra wave at the end of the QRS called an Osborne wave (or a J wave), which are highlighted by the blue arrows. There is also significant baseline artifact (best seen in V1), that’s called shivering artifact.
Final read: Severe bradycardia with shivering artifact and Osborne waves.
“Hey Doc! Look at the tele monitor quick! We have a rhythm change, I think he just went into Vfib!” you hear one of the techs call out.
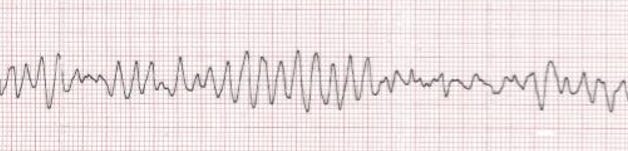
Well, that can’t be good. VFib is rarely good. Actually, I can’t really think of a time that I would be like, “Wow, thank goodness the rhythm is VFib. That’s good.” Anyway, let’s pause for a second to review accidental hypothermia and its management.
We’re going to attack a hypothermic resuscitation question-and-answer style. Most of these answers come from this excellent review of the management of hypothermia by Dr. Ken Zafren.
Let’s start with the most common question. Can some people be cold and dead? Or must everyone be warm and dead? Let’s start with the obvious, any patient with a fatal injury is allowed to be cold and dead. Think decapitation, open head injury with loss of brain matter, truncal transection, etc. If someone’s decapitated, it really doesn’t matter what their core temperature is; unfortunately, they are dead.
What if they’re pulled out of an avalanche? Reasons to terminate in the field include being buried for over 60 minutes with an airway completely obstructed by snow or ice.
Ok, we have none of those things. No avalanche and the patient’s head (and everything else) is still attached. But they’re super cold; core temp is 28℃. Now what? Well, if you’re in the field, take one full minute to check for signs of life. So, feel for a carotid pulse and check for any respirations (expect them to be slow and shallow). If there are any signs of life, don’t start CPR. If there aren’t, CPR is indicated.
Can monitors help us? Well, sort of. If you hook the patient up to a monitor and you see organized cardiac activity but can’t feel a pulse, it could be PEA or it could be an extremely faint pulse due to profound hypothermia. Make sure that the patient is hooked up to end tidal and use that to help you. If the end tidal is flat, that indicates cardiac arrest. If you see asystole, make sure that the gain is turned up as high as it will go to check for fine VF, as it common in hypothermia. If there is an organized rhythm other than VTach, CPR is only indicated if end tidal is flat or the POCUS echo shows no contractions.
If we do CPR, how long will it go on for? Well, about forever. Full neurologic recovery has been reported in patients with accidental hypothermia getting CPR for over 8 and a half hours!
How cold is futile? Tough to say. Case reports have shown that patients with a core temperature of 7℃ have been successfully resuscitated with good neurological outcome, so most algorithms do not have a “too cold” cut off.
Can I defibrillate someone this cold? Should I? Again, the answer is maybe. Case studies show that patients with a core temp less than 26℃ have been successfully defibrillated. It’s reasonable to make an attempt to defib someone under 30℃, but if it’s unsuccessful, don’t keep shocking, wait until they come up a degree or two until trying again. Patients with a core temp over 30℃ should follow standard ACLS defibrillation protocols.
What about intubation? This one is tricky. There is a risk of inducing VFib during intubation, but the risk is low enough that you should still intubate if it’s indicated. For medications, be aware that meds will likely be ineffective at a core temp less than 30℃. Also be aware that metabolism is slowed due to hypothermia, so expect these medications to linger in the system. You may see these agents work longer than normal, especially as the patient is rewarmed. If you decide to give medications for intubation, consider a lower dose, especially of paralytics.
What about ACLS drugs? The patient is arresting, should I push epi? Again, tough question. As would be expected, there isn’t great data on this. Drug metabolism is severely decreased in hypothermia, so if we give cardiovascular drugs (epi, vasopressin, amiodarone, etc) as we do CPR, they may build up to toxic levels in the tissues and, as the patient rewarms, can cause more harm than good. The review article (again, this paper by Dr. Zafren) recommends avoiding cardiovascular drugs with a core temp less than 30℃. Once the patient is between 30-35℃, use the standard dose of medication, but double the time interval between doses. So, for example, if you were to give epi every 3-5 minutes on a normothermic patient, give it every 6-10 minutes if their temp is between 30-35℃.
The patient is hypothermic and extremely bradycardic, should I float a pacing wire? NO! transvenous pacing is contraindicated due to extreme cardiac irritability. You can consider transcutaneous pacing if the patient is bradycardic and hypotensive in an attempt to allow for better circulation leading to better rewarming. Side note, if you choose to place a central line in these patients, be extra careful with the wire, these hearts are extremely irritable and the wire touching the myocardium can induce dysrhythmias.
Are there any labs I can use to help determine if resuscitation is futile? There are ZERO reported cases of a patient recovering with a potassium over 12 mmol/L.
Any other considerations? Yes, these patients should be emergently discussed with the ECMO team, as they are ideal candidates for ECMO and rewarming.
Case Wrap Up:
“That’s not good, we’re in ventricular fibrillation. Start CPR NOW!”
As the team initiates CPR, you recall there are some differences in the management of cardiopulmonary arrest in patients with hypothermia. You double-check to make sure active re-warming measures have been initiated; warmed (40-42℃) 0.9% saline IV, warmed (40-46℃) humidified O2 via nasal cannula, chemical heat packs in the groin/axilla, and that the Arctic Sun is running. You even consider placing a Foley for continuous bladder irrigation with warmed (42℃) fluids and chest tube thoracostomy with thoracic lavage because your center doesn’t have Extracorporeal Membrane Oxygenation (ECMO).
Pulling you out of your train of thought, the charge nurse asks, “Doc, do you want to give Epi?”
You confidently respond, “We shouldn’t use any vasoactive medications until the patient’s core temperature is at least 30℃, and once he hits 30℃, we need to double the normal dosing times of our ACLS medications until he’s above 35℃ because drug metabolism is decreased and protein binding is increased. If we get him warmed up and all those medications are circulating in his system, they could end up having a deleterious effect.”
She follows up with, “Well, he’s in VFib, do you at least want to shock him?”
You again confidently respond, “Yes, we can attempt defibrillation up to three times before he is above 30℃, but we shouldn’t do more than that.”
Unfortunately, the initial defibrillations are unsuccessful. You repeat the core temperature and it’s 31℃, so you begin to administer ACLS medications. The charge nurse notices the resuscitation team beginning to fatigue. She asks, “Doc, how long do you want to continue this resuscitation?” Before you can respond, the ER tech hands you a POCT Chem 7 that shows a potassium of >12 mg/dL.
You dejectedly respond to the charge nurse, “We should stop now. His core temperature is above 30℃, his potassium is greater than 12, and he hasn’t had an organized cardiac rhythm since he got here. All of the guidelines that I’m familiar with suggest we cease resuscitation efforts.” Giving the entire team the chance to voice any concerns, everyone agrees that although it was a valiant effort, continued resuscitation is unlikely to produce a favorable neurologic outcome or even ROSC for that matter.
Recap:
- Some patients are allowed to be cold and dead!
- Think patients with an obvious, nonsurvivable injury. If the patient’s torso is transected, they aren’t coming back
- Start CPR and get the patient hooked up to both a cardiac and end tidal CO2 monitor.
- Cardiac monitors aren’t always trustworthy at hypothermic temperatures, use the end tidal CO2 to help you recognize true cardiac arrest
- POCUS Echo can also help differentiate PEA from a very weak pulse
- Defibrillation under 30℃ isn’t likely to be effective. You should still try!
- Protocols differ, some recommend 1 shock at max output while others recommend 3 shocks and then holding further until the patient is warmer
- If you’re thinking of using ACLS drugs:
- Core temp <30℃, best to hold off on drugs for now
- Core temp 30℃ – 35℃: Ok to give drugs, but double the time interval
- Core temp >35℃: Standard ACLS protocol
- Remember, transvenous pacing wires are contraindicated in hypothermia
- No hypothermic patient has been successfully resuscitated with a potassium over 12 mmol/L
- Here is a fascinating case report of a pediatric patient with an initial core temperature of 7℃ (45℉) who was submerged for 147 minutes and made a good recovery! Great work team Geisinger!
- Thank you Drs. Kessler and Merrill for your help with this write up!
Hit me up with any questions,
Lloyd