Written by Joshua Belfer
![]()
Meningococcal disease is a rapidly progressive infection associated with high mortality that often begins with nonspecific symptoms; early recognition, early antibiotics, and aggressive resuscitation are critical to improving outcomes.
A disease that punishes delay
Invasive meningococcal disease (IMD), caused by Neisseria meningitidis, remains one of the most dangerous infectious diseases encountered in the ED. Although relatively uncommon, IMD carries significant morbidity and mortality rates, up to 80%. Early disease often mimics benign viral illness, leading to diagnostic delay with catastrophic consequences. IMD encompasses a spectrum of illness, most commonly presenting as meningitis, meningococcemia, or both.
Presentation:
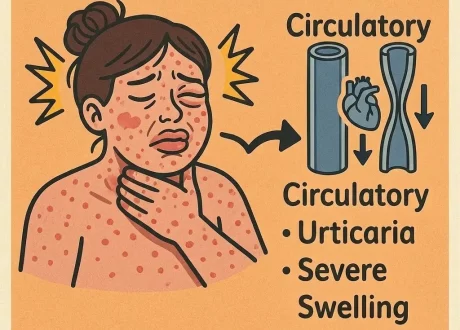
Early (first 6–9 hours) meningococcal disease has nonspecific symptoms that resemble a flu-like illness: fever, chills, myalgias, nausea, and vomiting. As the disease progresses—often quickly and unpredictably—meningitis can present with the classic triad of fever, neck stiffness, and altered mental status (only seen in 44–66% of cases). A nonblanching petechial or purpuric rash is concerning for meningococcemia but can be absent early.
Workup:
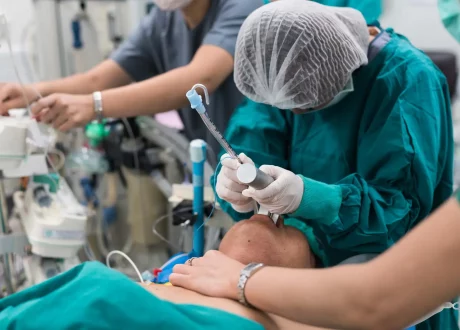
While diagnosis should not delay treatment, lumbar puncture remains the diagnostic gold standard for meningitis. Blood cultures should be obtained, and labs may show leukocytosis, thrombocytopenia, coagulopathy, and elevated lactate. CT head imaging should precede LP in patients with risk factors for herniation but should not delay antibiotics.
Management:
IMD is a time-critical diagnosis, and optimal management relies on early recognition. Strict isolation and droplet precautions should be initiated, and antibiotics should be started ideally within one hour of recognition. Therapy should include a third-generation cephalosporin and, in areas with pneumococcal resistance, vancomycin. Aggressive resuscitation with fluids and, if needed, vasopressors is recommended, along with adjunctive corticosteroids. Chemoprophylaxis should be initiated for all close contacts.
Pearls and Pitfalls:
- Early IMD often looks viral.
- Not all patients will have the classic meningitis triad, and Kernig and Brudzinski signs have poor sensitivity (2%).
- Delaying antibiotic therapy until the LP is completed is the most common error in the ED management of meningitis.
How will this change my practice?
Meningococcal disease is rare enough that we may only see a handful of cases—or none—over our careers. Be cautious, especially with the febrile patient who initially looks “viral” but worsens. When suspected, early initiation of antibiotics is crucial and can be life-saving. We typically wait for the cultures to be drawn before starting antibiotics, but when meningococcal disease is on the differential, it’s time to ignore that dogma.
Source
High risk and low incidence diseases: Meningococcal disease. Am J Emerg Med. 2026 Jan;99:114-122. doi: 10.1016/j.ajem.2025.09.031. Epub 2025 Sep 18. PMID: 41016083.