Written by Joshua Campbell

Relative thoracic distention pattern seen on capnography during cardiac arrest may have a negative impact on blood pressure and cerebral perfusion. Here’s how to recognize and fix it.
If you’re not a subscriber yet, become a JournalFeed member today! Since you need to know these ETCO2 patterns, the link to the full text is here. Subscribe. Save time. Get the Spoon Feed!
Why does this matter?
Yesterday, we learned compression depth has a bigger impact on ETCO2 variability than compression rate. We know the capnography number matters, but are there ETCO2 patterns during chest compressions that might help us optimize CPR quality as well?
What do we do with the CO2?
In the management of cardiac arrest, high-quality CPR is the most vital part of resuscitation. Capnography has become a very useful tool in assessing progress during resuscitation, but chest compressions during CPR influence the CO2 waveform and complicate interpretation. The authors of this study aimed to classify different CO2 patterns during compressions that would be useful to recognize during CPR and the effects on circulation.
Three capnogram patterns were described: (see figure)
- A) Intrathoracic airway closure: oscillations due to chest compressions and decompressions are small or absent (bad).
- B) Thoracic distension: oscillations due to chest compressions and decompressions are limited or absent at the beginning of the expiration phase and resume after a few chest compressions due to overdistended lung volumes decreasing back to below functional residual capacity, FRC (bad).
- C) Regular pattern: oscillations due to chest compressions and decompressions are clearly visible during the entire duration of the expiration phase (good!).
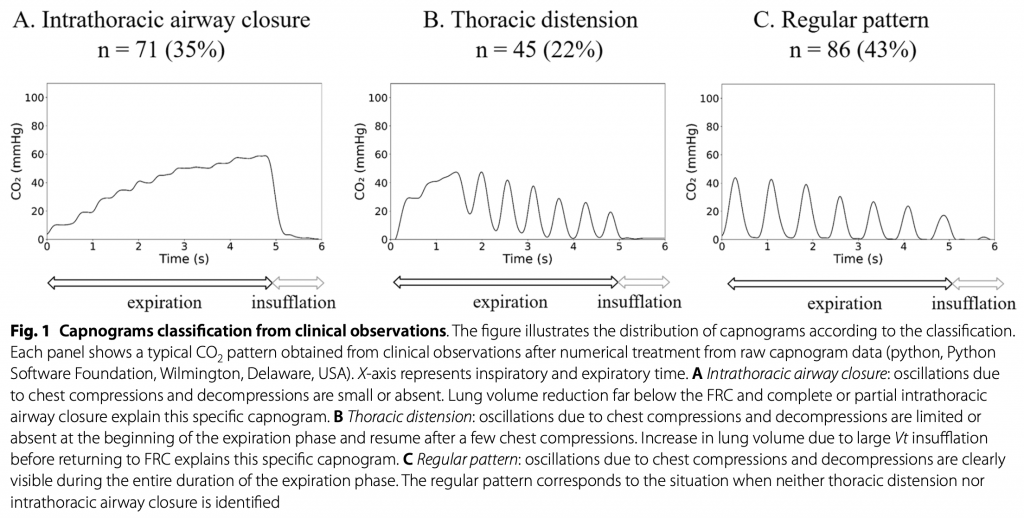
Here is the way tracings would actually look during arrest while performing compressions.
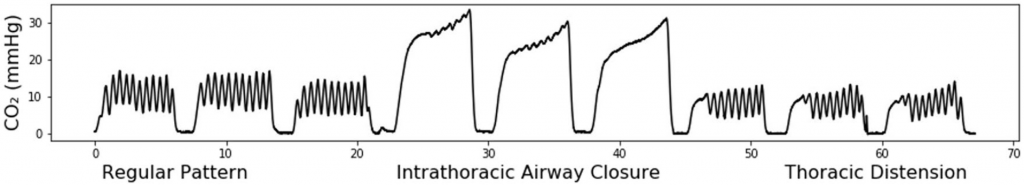
The authors analyzed 202 out-of-hospital cardiac arrest patients who were intubated with standardized ventilator settings, reproduced different CO2 patterns in human cadavers with CPR, used a mechanical bench with simulation of CO2 production, and used a pig animal model to assess varying tidal volume (Vt) influences on capnogram patterns during CPR.
This study found that intrathoracic airway closure, thoracic distension, or regular pattern can be reliably identified by the capnogram analysis. In the OHCA patients, 35% showed airway closure, 22% thoracic distention patterns, and 43% regular pattern. In the animal experiment, greater thoracic distension was inversely correlated with cerebral perfusion and arterial blood pressure, while no correlation was found with tidal volume.
There are several limitations to this study, including capnogram analysis only during continuous chest compressions, only one ventilatory cycle soon after intubation was analyzed, and factors related to animal studies. However, this moves us closer to utilizing capnography during CPR to making dynamic changes to improve resuscitation. We now know capnogram patterns can be recognized during CPR, and this has the potential to help us optimize CPR quality.
Editor’s note: There are specific actions for each bad pattern. 1) For intrathoracic airway closure, ensure chest recoil between compressions and try adding PEEP. 2) For thoracic distension, try reducing tidal volume. ~Clay Smith
Source
A novel capnogram analysis to guide ventilation during cardiopulmonary resuscitation: clinical and experimental observations. Crit Care. 2022 Sep 23;26(1):287. doi: 10.1186/s13054-022-04156-0.