Apr 27, 2026
Contributor: Alec Coston, MD
Educational Pearls:
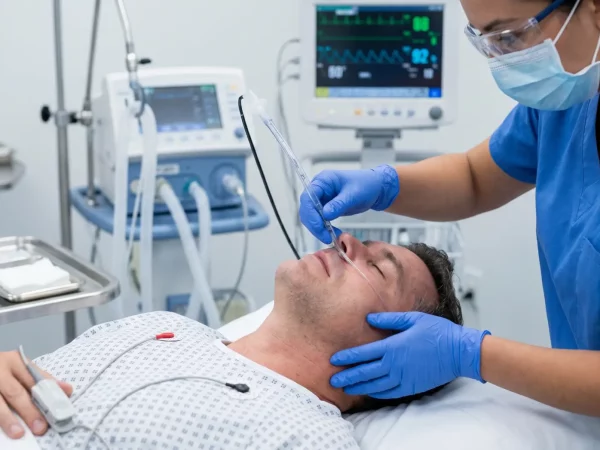
What are nasal intubations and when do we use them?
-
Nasal intubations function similarly to oral intubations with the end goal of passing an endotracheal tube (ETT) through vocal cords and into the trachea to allow for a patent and secure airway, but differ in the main access point for the ETT (nare v.s. mouth).
-
Nasal Intubations are seldom preferred to oral intubations as they carry risk for inducing bleeding from trauma to the nasal passages.
-
Indications for nasal intubations include:
-
Anatomical abnormalities that may make access through the mouth difficult (i.e. tumors, macroglossia, or rare dental hardware that clenches the jaw shut).
-
Physiological states such as severe angioedema.
-
-
Nasal intubations are often done with the patient awake and could be advantageous if the patient is presenting in a severely hypoxic state such that prolonged hypoxia in a traditional RSI protocol may be detrimental.
-
A 2023 retrospective analysis in Germany found that nasal intubations were associated with requiring less sedation than oral intubations and had more spontaneous breathing during hospitalization than oral intubations.
How is a nasal intubation performed?
-
Consider the use of an anxiolytic medication such as versed to calm the patient down but not fully sedate them.
-
If there is adequate time without immediate patient compromise, consider glycopyrrolate to reduce airway secretions and dry up the mucous membranes.
-
Consider the use of Afrin or other local vasoconstrictor in target nare to minimize epistaxis.
-
Use 5% lidocaine ointment and lubricate an NPA and place it into the target nare. This will allow for local anesthesia as well as help to open up the nare slightly more.
-
Take 5% lidocaine ointment and place it on a tongue depressor and move it around the back of the tongue, allowing it to further anesthetize the oropharynx.
-
Remove the NPA and atomize/nebulize 4% lidocaine liquid into the nare and into the oropharynx for further anesthesia.
-
Insert the ETT without the bronchoscope through the nare and allow it to pass about 10 cm until visible in the oropharynx. This allows for a “clean” plastic tunnel to pass the bronchoscope through.
-
Advance both the ETT and bronchoscope, spraying lidocaine through the bronchoscope while advancing to allow for continued numbing.
-
Pass the ETT through the cords and inflate.
-
At this point, stronger sedation medications such as ketamine and propofol may be considered but the use of a paralytic like succinylcholine and rocuronium may not be needed to allow the patient to maintain their own negative pressure ventilation.
Which nare is the best to go through?
-
Most patients will have their right nare be the best (away from the septal deviation) according to a meta-analysis by Tan et al.
-
The right nare was generally associated with less epistaxis and lower intubation times.
-
However, do not always default to the right nare, and test which nare is more patent by occluding one nare at a time and assessing which one is less resonant (less resonant = more patent).
Key Takeaway?
-
Nasal intubations are rarer than oral intubations and can be more technically difficult, but may offer advantages in patients with difficult oral airways, but should never be first line.
References:
-
Grensemann J, Gilmour S, Tariparast PA, Petzoldt M, Kluge S. Comparison of nasotracheal versus orotracheal intubation for sedation, assisted spontaneous breathing, mobilization, and outcome in critically ill patients: an exploratory retrospective analysis. Sci Rep. 2023;13:12616. doi:10.1038/s41598-023-39768-1
-
Tan YL, Wu ZH, Zhao BJ, Ni YH, Dong YC. For nasotracheal intubation, which nostril results in less epistaxis: right or left?: A systematic review and meta-analysis. Eur J Anaesthesiol. 2021;38(11):1180-1186. doi:10.1097/EJA.0000000000001462
-
Holzapfel L. Nasal vs oral intubation. Minerva Anestesiol. 2003;69(5):348-352.