![]() ECG Teaching Cases
ECG Teaching Cases
Mar 25, 2026
“Hey, Doc, can you pick up the phone? There’s a call for you on line 2,” you hear Shannon, your charge nurse, call out.
“Uhhh? Sure? Who’s calling?” you ask her.
“It’s the 9-1-1 center, Doc. They just got a strange call and wanted to give us a heads up about a patient who may be coming in. Grab a phone, I’ll listen too.”
“Ok, sure,” you say as you pick up the phone, “Hello! How can we help?”
“Hello Doctor, this is the 9-1-1 center. We just got a strange call from one of the local park staff and wanted to give you a heads up. According to the park supervisor, a young woman was driving her car near the park when she suddenly stopped in the middle of traffic. She ran out of her car and flagged down a park ranger. She told him that she had overdosed on her medications in a suicide attempt but regrets it and needs help. She says she was trying to drive to the hospital but got too weak and couldn’t make it. Immediately after talking to the ranger, she went unresponsive. According to him, she has a weak pulse, is breathing on her own, but is completely out. I’ve dispatched Medic 1529 to their location. That park is just down the road from you, so I doubt the medics will have time to give you a heads up about her. If I had to guess, ETA is less than 5 minutes to your door. Thanks, Doc, good luck!”
You and Shannon exchange glances. “Oh boy, here we go again,” you tell her, “Let’s get room 9 ready to go and get RT too, sounds like she may need a tube. As soon as she gets here and we get a name/MRN, I’ll talk to Scott and see if he can work some pharmacy magic and tell us what meds she may have taken. Thanks Shannon!”
“Doc, EMS rolling in! They’re in a hurry!” you hear Shannon call out. “Hey Medic 1529, head to bed 9, Doc will meet you there.”
You see the medics unload the stretcher quickly and head to bed 9. They are actively bagging the patient. “Hey Doc, this is the young lady the 9-1-1 center called you about. She ran up to a park ranger after an overdose. We found her ID in her car, so at least we have a name for you. She is super sick and getting worse. Right as we pulled in, her breathing got even more shallow so we started assisting her. HR is in the 40s, BP is 70/32, Resp Rate is 9, SpO2 is 91%, Afebrile. Glucose is 120. There was no change with naloxone. As you can see, she has a GCS of 3, has mid-range pupils and she’s pretty hyper-reflexic despite her decreased muscle tone. That’s about all we know.
“Thanks Medic 1529. Shannon, let’s get set up to intubate, but we’ll need to fix that blood pressure first. Let’s give 2L IVF wide open and have pressors on standby. Scott, did you get a chance to look her up?”
“Yeah, sure did!” Scott tells you. “She has a prescription for Baclofen and Clonidine. You look a little busy right now so I’ll put out a stat call to Tox.”
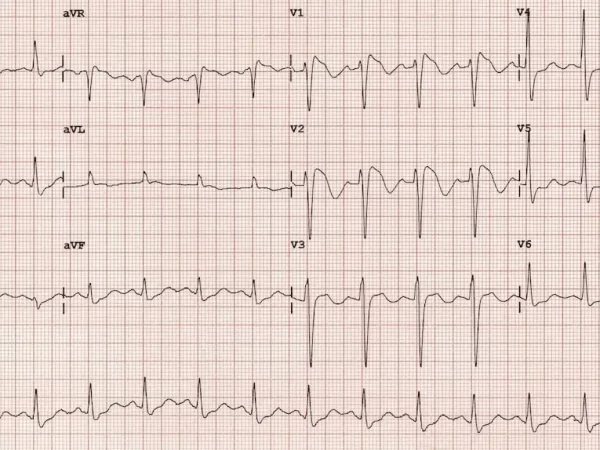
“Oh, hey Doc, this was the EKG we got on her in the rig on our way over before she got worse,” you hear the medics tell you before they leave.
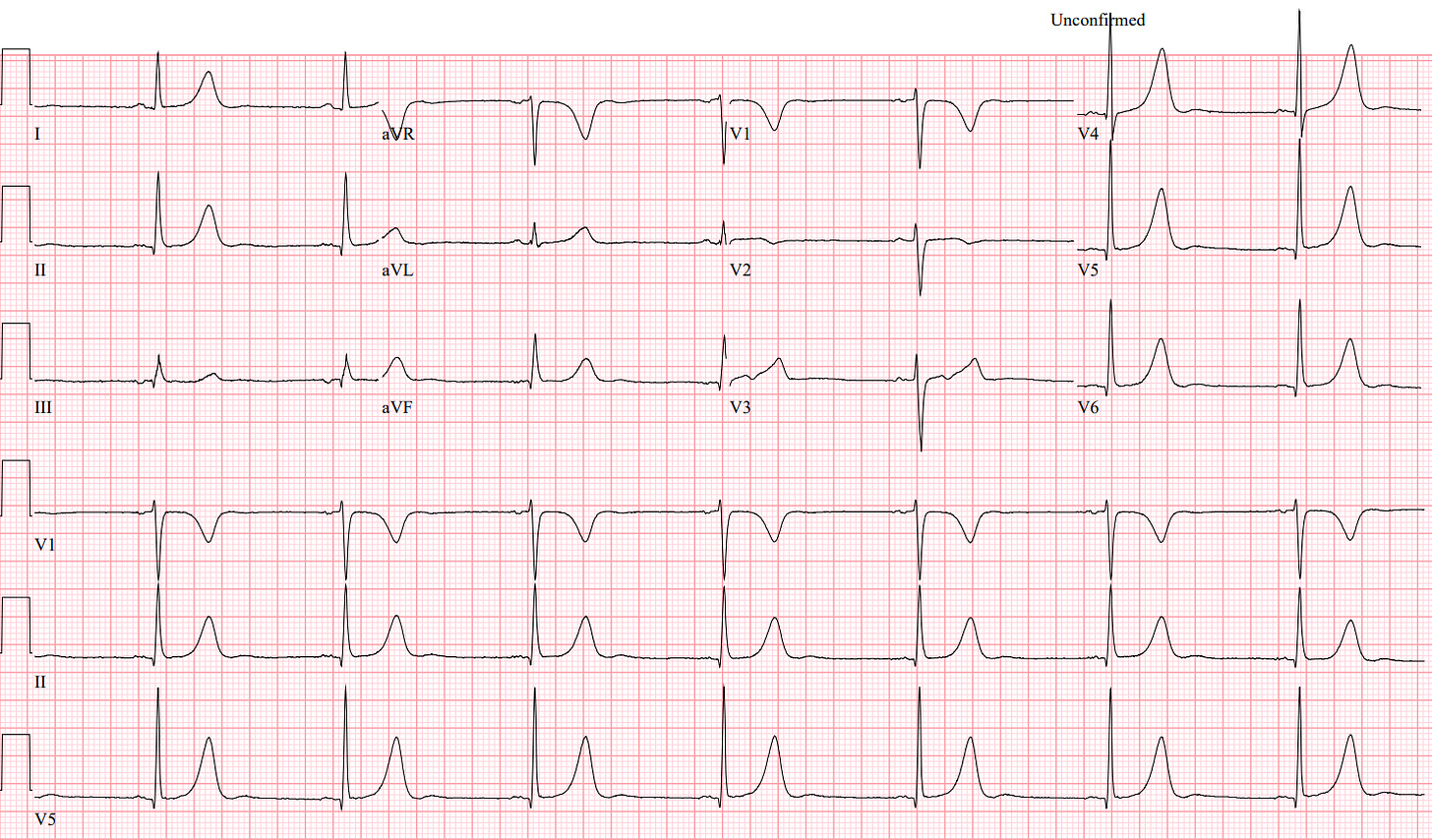
Rate: 42 beats per minute
Rhythm: Sinus rhythm
Axis: Normal
Intervals; All look to me. Normal PR, QRS narrow, QTC looks good too
Morphology: pretty good overall
Final read: Sinus bradycardia
“Hey, Doc, get your head out of that ECG and take a look at the repeat vitals!” you hear Shannon call to you. “We haven’t ever started the fluids yet and her BP re-cycled to 180/102. We checked it twice and it gave us pretty much the same number.”
“That’s really weird… Oh no! She’s seizing. That’s bad. Scott, I need some Ativan now! Please.”
You push Ativan and eventually the seizure stops. You manage to get her successfully intubated but her blood pressures are all over the place, ranging from severe hypertension to worrisome hypotension. Right as you’re trying to puzzle through what to do, you hear a knock on the door.
“Hey there! I heard you had a really sick overdose patient, and I was in the building so I thought I’d drop by and see how I can help!” you hear the familiar voice of Dr. Bill Boroughf, toxicologist extraordinaire!
“Yeah, man,” you say, “this one’s really weird! At first, she was alert and driving. And then, she was comatose, bradycardic and hypotensive. It all seemed consistent with a big clonidine ingestion. But now… this” you say with a confused face motioning towards the intubated, tachycardic, hypertensive and slightly twitching patient. “She can’t figure out if she wants to be hypotensive or hypertensive, bradycardic or tachycardic, comatose or seizing! She’s been all the things over the past 10 minutes. What the heck is going on here?”
“Yup,” says Bill, “definitely not a clonidine overdose.”
“Thanks for that,” you say glibly. “Those two extra fellowship years were clearly worth it…”
“What are the chances this lady is on baclofen?” Bill asks
“Wait, what? How’d you know?”
“There are only two agents that will play this game with her vitals. One is phenibut, an anxiolytic from the 1960s Soviet space program that is currently misrepresented as a “dietary supplement” in the interwebs. The other is baclofen.”
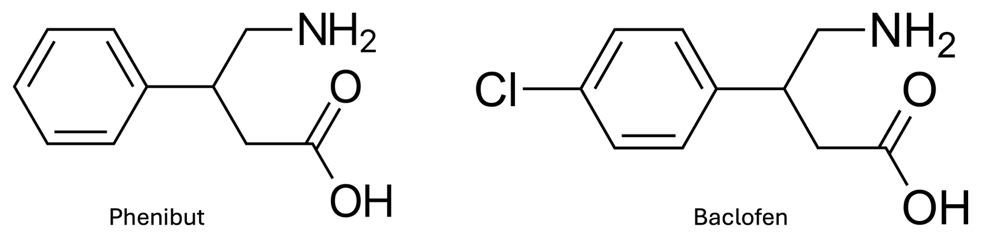
(How could a tox write up not include at least one chemical drawing…)
“Ok, Dr. tox nerd, I know a thing or two about baclofen, myself. It’s a muscle relaxer, but unlike the other messy relaxers, this one works solely on GABA, the sedating neurotransmitter, just like benzos. So, why doesn’t she look like a benzo overdose?”
“Ah, yes. Welcome to the weird and wonderful world of GABAB! That’s “B” as in “better buckle up for a bumpy ride, bro!”
“Ok, I’ll bite,” you say. “What’s GABAB and why does it matter in the management of our friend here?”
“I’ll try to be brief (well, as brief as a tox nerd can be, at least). It’s true that GABA is our favorite inhibitory neurotransmitter. It binds to receptor sites and hyperpolarizes the neuron, which makes it harder to fire. Hence: sedation. And this is exactly how benzos, barbiturates, and booze work. But, importantly, these all work on a GABAA receptors.
“And GABAB?” you ask.
“GABAB receptors are located on pre- and post-synaptic regions, which is key to its toxicity. When post-synaptic GABAB receptors are activated, you get the usual post-synaptic signal inhibition, which causes sedation, similar to our benzos. However– and this is important–stimulation of pre-synaptic GABAB receptors results in inhibition of the release of inhibitory neurotransmitters. Think of it like a traffic signal that defaults to green unless some dude is actively pushing a button to turn it red. It’s his job to regulate who stops and who goes. But then baclofen comes along and knocks the guy out! Now, he can no longer hold the STOP button, and everything goes all green-light all the time.”

“Ahh,” you say. “It’s like a physiological double-negative: Inhibition of inhibition causes excitation. So that explains the hypertension, tachycardia and seizures. But what about the sudden hypotension and bradycardia that randomly develop?”
“Ah yes, remember that receptor binding is not permanent; drugs bounce on and off receptors with varying frequency resulting in waxing and waning of effects. Baclofen is a particularly fickle jerk. When it’s not knocking out presynaptic inhibitory traffic controllers, it is fully hyperpolarizing the post-synaptic GABAB receptors, leading to profound hypotension and coma.”
“Thus, baclofen overdose has a classic picture of rapidly alternating agitation/sedation, bradycardia/tachycardia, and most problematically, extreme hypotension and hypertension– especially in high doses ( i.e. >200 mg). Cases have been reported of patients swinging back and forth between 200s/100s to 50s/30s and back again over the course of an hour.”
“This sounds like a set up for a wild ride, indeed. So how do we manage all of this?” you ask, looking at the monitor as your patient’s blood pressure is starting to drop again.
“Drips,” Dr. Bill says. “Lots of drips. One of the key principles for management of baclofen overdose is to anticipate these massive swings and employ your rapidly-titratable infusions to both increase and reduce blood pressure. The higher the overdose, the greater the risk of extreme autonomic instability. The agents you choose should be based on your familiarity and local availability, but they should be rapidly acting and short-lived. Most literature recommends esmolol or nicardipine for critical hypertension and norepinephrine (noradrenaline) for fluid-unresponsive critical hypotension. Things are typically the most challenging during the first 4-6 hours after the overdose. After that, baclofen apparently gets tired of playing games and hypotension and coma usually predominate. Just for extra fun, all of this can be associated with recurrent seizures which can progress to status epilepticus. Thus, intubation is also commonly needed.
Fun(?) fact: In high doses, the baclofen-associated coma can be so profound as to mimic brain death for days. A handful of cases have reported baclofen overdose patients who were declared “brain dead” who then woke up after being listed for organ donation procurement, some with good neurological function! Thus, brain death determination in baclofen-associated overdose should be made extremely cautiously and should follow published recommendations and/or in partnership with your local tox nerd.
Case Wrap up:
“Hello? Dr. ICU? Hey, it’s the ER again. Boy, do I have a case for you. 47-year-old female coming in after a baclofen and clonidine overdose. Blood pressure and heart rates have been all over the place. Due to her mental status we had to intubate her. We have several drips running, including esmolol and norepi to help manage her autonomic instability. She’s very rapidly, and unpredictably, alternating between tachycardia/bradycardia and hypertension/hypotension. Last seizure was 25 minutes ago. We have Dr. Boroughf on the case too. He said he’ll come up and run you through what to expect for the next couple of hours… You accept? Great, thanks!”
Recap
- Baclofen overdoses are extremely challenging to manage
- Expect extreme autonomic instability – these patients will be unpredictably hypertensive, hypotensive, tachycardic, and bradycardic
- Involve your toxicology colleagues early!
- You’ll need multiple drips to manage these patients, ask your pharmacy friends for help too
- Expect to use rapidly titratable drips, such as esmolol, nicardipine or norepinephrine
- Baclofen overdoses are most challenging to manage for the first 4-6 hours, as this is when the autonomic instability will be the most extreme
- Be careful declaring brain death in these patients, in high doses, the baclofen-associated coma can be so profound as to mimic brain death for days
- Here are the guidelines for brain death again and, if possible, talk to a toxicologist
- Thank you again Dr. Bill Boroghf for your expertise and insights! And please take a look at his substack, The Thing About Poison, with Dr. Bill Boroughf for more excellent toxicology knowledge!
Hit me up with any questions,
Lloyd
Heading to ICEM 2026 in Hamburg, Germany this year? I’ll be speaking at the Emergency Cardiology Challenges Workshop on 9 June 2026 with Dr. Amal Mattu and friends! Come say hi!
**Looking for a dynamic guest lecture on Emergency Cardiology for your Grand Rounds? Reach out here for a lecture request by Dr. Tannenbaum. If you have reached out already, I have emailed you back. If you haven’t gotten it, please message me directly on Substack or just reply to this email.**
_________________________
Lloyd Tannenbaum, MD