***This is a case that I found particularly challenging. Joining me today to discuss the diagnosis and management of cardiogenic shock is my friend and mentor, Dr. Brit Long. Dr. Long is a professor of emergency medicine at the University of Virginia and an internationally recognized author and educator. He’s one of the editors-in-chief of emdocs.net and an amazing colleague to work with clinically. I hope you learn as much from this as I did.***
“Can I get some help in here please!” you hear your senior resident call out.
That can’t be a good sign. You and your charge nurse, Shannon, hustle over to room 9 to see what’s going on.
“This is Mrs. Rojas,” your resident calls to you. “She’s a 78 year old female coming in with shortness of breath and lower extremity swelling. Triage called me to come take a look at her and I had them bring her right back to one of the resuscitation rooms. She looks terrible. Heart rate is in the 150s, blood pressure in the 70s/30s, respiratory rate is in the 20s, oxygen saturation is 87% on room air. At least she isn’t febrile, though.”
“Mrs. Rojas, how are you feeling?” You ask her.
“Not so great, doctor. I’m so tired, I can barely get up out of bed anymore. And I’m retaining so much fluid, I know something is wrong. I’ve had congestive heart failure for the past 25 years, and I’ve never had an exacerbation like this before. I try and walk to the bathroom and I’m so short of breath, that I can barely make it.”
“Here’s the ECG, Doc. I’ll get a second point of IV access on her and draw a rainbow of labs. I also called X-ray to come shoot a quick chest. Anything else you need?” Shannon asks you.
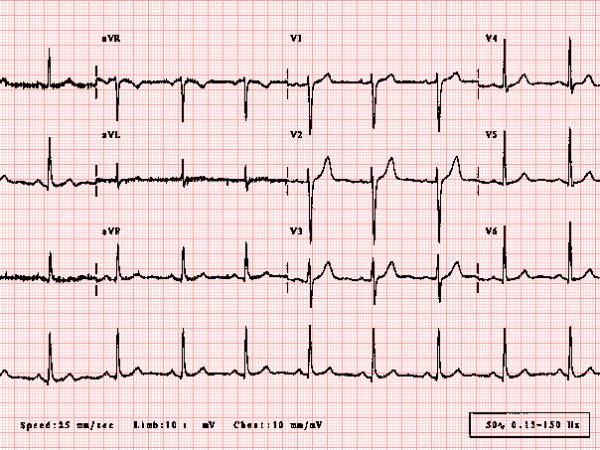
“I think that covers it for now,” you say, handing the ECG to your resident. “Tell me, what do you see on this ECG?”
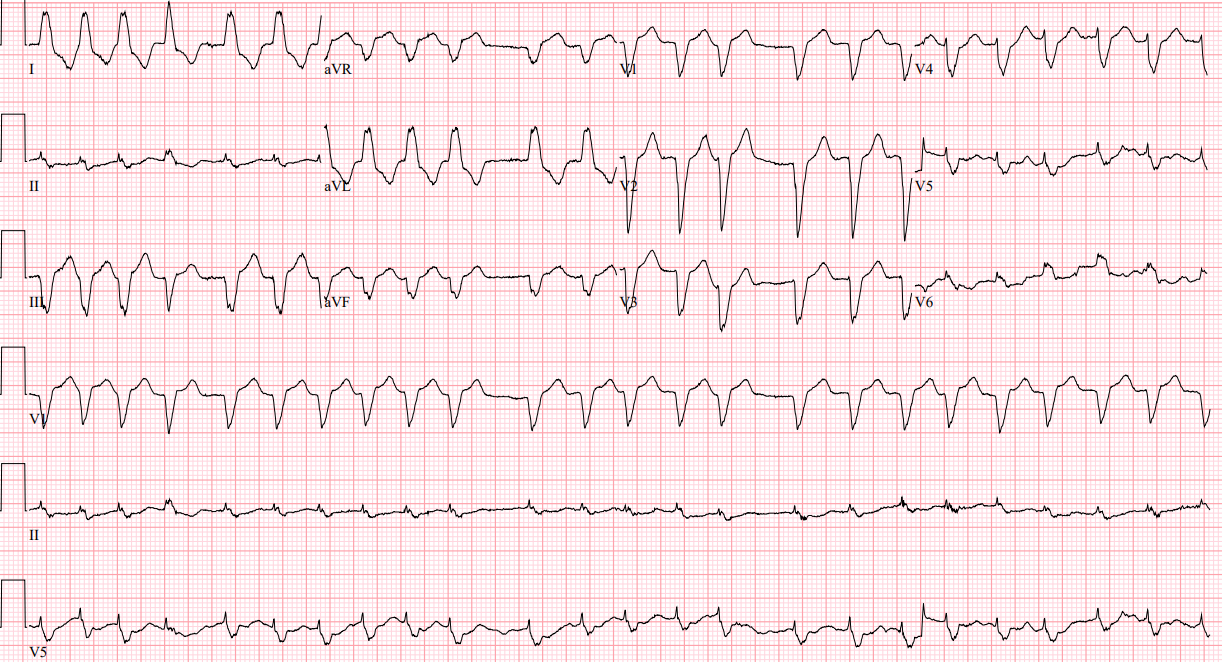
Rate: 144 beats per minute
Rhythm: Irregularly irregular, atrial fibrillation (AF)
Axis: Left axis
Intervals: no PR interval, widened QRS, QTc looks ok
Morphology: Left bundle branch block is present
Final Read: AF with a left BBB
“Very good!” you tell the resident. “Now, what’s the plan?”
“Ummmm. Well… This looks like a heart failure exacerbation. Mrs. Rojas has extremely swollen legs, crackles up her back when you listen to her lungs, and her POCUS shows a severely dilated IVC. But her blood pressure is really tripping me up. I definitely shouldn’t use nitroglycerin with that blood pressure. Can we use BPAP with hypotension? And she probably needs resuscitation too. But with her being so volume overloaded, I don’t want to give her any more fluids. What’s the best pressor for hypotensive heart failure? I’m a little lost.” She tells you.
Great Questions. Let’s dive into the finer details of how to manage these complex patients!
Dr. Long, take it away!
This is a complex patient who is acutely decompensating. We have to act quickly, but at the same time, we have to consider the underlying pathophysiology. She is hypotensive with respiratory distress, has AFib with rapid rate, and is volume overloaded, all in the setting of what is likely hypotensive heart failure. This is a complicated patient with several underlying issues. For any critically ill patient, step back and remember the ABCs. We need to address her respiratory distress, hypoxemia, hypotension, and heart rate.
First, I’m going to start a norepinephrine infusion and place her on BPAP or CPAP as soon as possible (this is an oxygenation issue, so CPAP is fine, but I prefer BPAP) to address the hypotension and respiratory status. She’s volume overloaded on exam, so fluids are not the best idea. Norepinephrine is the best option for this patient and her hypotension. It’s often the fastest vasopressor most EDs can set up, and it’s likely the most effective inopressor for this specific patient. If there’s any delay in starting the norepinephrine infusion, I’m going to make push dose epinephrine at the bedside.
Also, patients may have an issue with the BPAP mask, and if they do, I’m going to give small doses of ketamine (20 mg IV aliquots) until they’re dissociated (place on capnography and treat this as a sedation) and more comfortable.
Of course I have to talk about POCUS! We are emergency clinicians after all. Take a look with the US at her heart and lungs. My main questions on US are:
- What do the LV and RV look like (squeeze, size, ratio)?
- Is there a pericardial effusion?
- Is there a clot?
- Are there B lines/pulmonary effusion/lung sliding?
If you feel comfortable with US, you can also take a look for valvular issues like stenosis/regurgitation, but that’s extra credit.
Once I have her on BPAP and norepinephrine running, I’m going to reassess. If the heart rate remains elevated, this is a patient I’m leaning towards cardioverting with etomidate 0.1 mg/kg IV and electricity (200J biphasic). In general, management of heart failure focuses on decreasing afterload and preload while improving inotropy, but we can’t readily do this in the patient with AF and soft pressures. That’s because we can’t decrease afterload or preload if they are hypotensive. We do want to increase inotropy, but we need to avoid increasing chronotropy if possible because of the rate issues. Where does this leave us? In patients who are unstable with AF and elevated rate (> 150s), get them back to a normal rhythm with electrical cardioversion, which is supported by the 2023 AHA guidelines.
Even if this patient has improved pressures and perfusion but her rate remains elevated, I’m still going to move towards electrical cardioversion. Normal sinus rhythm with an atrial kick will increase the cardiac output by about 10%, and slowing the rate with cardioversion will allow for improved filling of the ventricles.
I’m also going to anticoagulate with low molecular weight heparin if the patient is not on a DOAC. The risk of embolism in patients with CHF and AF is extremely high, and these patients need anticoagulation. If the patient is stable and they have decompensated HF, amiodarone 150 mg IV or digoxin 0.5 mg IV are other options to consider.
Avoid beta blockers (metoprolol) or non-dihydropyridine calcium channel blockers (diltiazem) if the patient is hypotensive and has a depressed EF (or if you’re not sure of their EF).
What if the patient does not have AF with rates in the 140s-150s, but she’s hypotensive, volume overloaded, and hypoxic?
That’s a great question. I’m still starting norepinephrine and BPAP while taking a look with POCUS. If I see B lines and poor EF with hypotension, this is concerning for cardiogenic shock. If it’s an RV issue, that’s a different story (and deserves its own post). Cardiogenic shock is a syndrome of reduced cardiac output resulting in hypoperfusion and end organ injury. Not a condition associated with great outcomes… Mortality rates approach 40%.
For some extra, bonus science, there is a classification system for this used by the American College of Cardiology and Society for Cardiovascular Angiography and Interventions (SCAI) ranging from those at risk of developing cardiogenic shock (SCAI A) to acute or impending circulatory collapse (SCAI E). This system takes into account exam, labs, and hemodynamics. On your exam, pay attention to vital signs (SBP, MAP, shock index, RR, saturation), extremities (temperature, edema, pulses), work of breathing, mentation, and lung auscultation (also US). Other than the ECG, order CBC, electrolytes, renal/liver function, troponin, BNP (not helpful acutely but will assist my inpatient colleagues), VBG/lactate, and potentially a TSH. We’re looking for evidence of end organ injury with increases in serum creatinine, LFTs, lactate, troponin, and acidosis on these studies. Pay attention to the ECG for evidence of occlusive myocardial infarction, as these patients need emergent reperfusion.
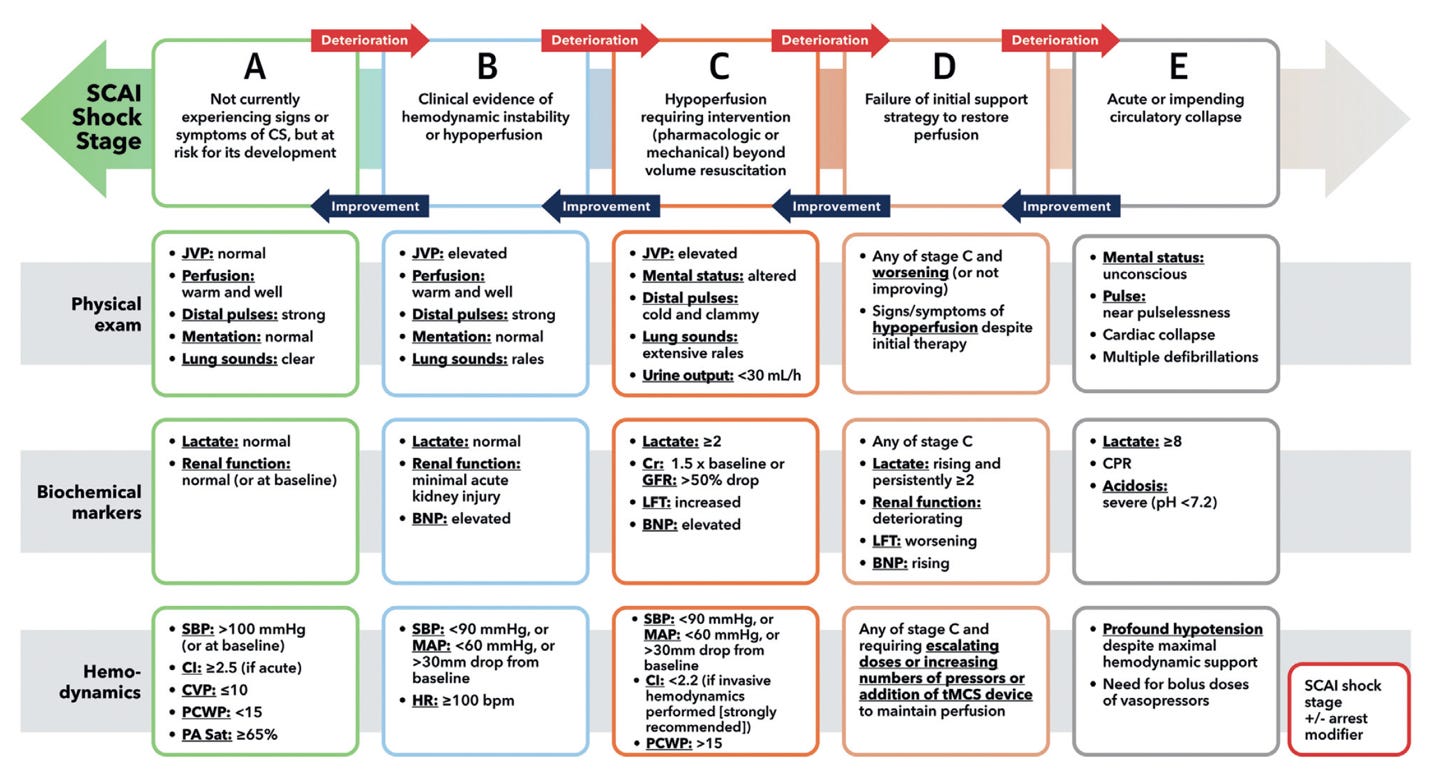
Ref: https://www.jacc.org/doi/epdf/10.1016/j.jacc.2025.02.018
Management of cardiogenic shock is based on improving perfusion and cardiac output. There are no high quality data specifying a hemodynamic target. This is where your clinical acumen comes into play; consider mentation, MAP, RR, HR, urine output (you should place a Foley and track urine output at some point), and peripheral perfusion.
To improve perfusion in patients with cardiogenic shock, start with norepinephrine; this is an inopressor that will support cardiac output and systemic vascular resistance. Dobutamine and milrinone are inodilators that can drop pressures if used in isolation. If hypoperfusion remains an issue despite norepinephrine, then reach for dobutamine or epinephrine.
When to intubate is always an important question. Start with NIPPV like BPAP or CPAP, but this is not the patient where you can start on BPAP and then walk away. If they are not improving, you need to intubate. If you’ve started BPAP, you’re preoxygenating already. I like etomidate and rocuronium for my intubation medications. Definitely have norepinephrine running if you are going to intubate and expect peri-intubation hypotension.
The final issue is that you need to speak with cardiology as soon as possible for these patients, and they likely need transfer to a tertiary care center. Patients may need mechanical circulatory support devices and emergent surgery.
Case Wrap up:
You start Mrs. Rojas on a norepinephrine drip and manage to get her MAP above 60. At that point you place her on BPAP and give cardiology a call. The cardiology team sends their fellow down to take a look while you place a call to the ICU for admission.
Recap:
- Go back to the basics: A, B, C.
- For cardiogenic shock, the goal is to improve perfusion and cardiac output.
- Norepinephrine is the first line inopressor, and start on NIPPV. Intubate if they do not improve or worsen.
- Labs, ECG, POCUS are vital. Look for end organ injury. On POCUS, look at LV and RV, pericardial effusion, clot, B lines/pulmonary effusion/lung sliding.
- If the patient is in AF with RVR and soft pressures, electricity is the treatment.
- If you need to intubate, expect peri-intubation hypotension and have pressors running before pushing induction medications
- Thank you Dr. Long for your insights and expertise!
Hit me up with any questions,
Lloyd
Heading to ICEM 2026 in Hamburg, Germany this year? I’ll be speaking at the Emergency Cardiology Challenges Workshop on 9 June 2026 with Dr. Amal Mattu and friends! Come say hi!
**Looking for a dynamic guest lecture on Emergency Cardiology for your Grand Rounds? Reach out here for a lecture request by Dr. Tannenbaum. If you have reached out already, I have emailed you back. If you haven’t gotten it, please message me directly on Substack or just reply to this email.**
_________________________
Lloyd Tannenbaum, MD
APD, EM Residency
Geisinger Wyoming Valley
Selected References from Dr. Long:
- Writing Committee Members; Joglar JA, Chung MK, Armbruster AL, et al. 2023 ACC/AHA/ACCP/HRS Guideline for the Diagnosis and Management of Atrial Fibrillation: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2024 Jan 2;83(1):109-279. doi: 10.1016/j.jacc.2023.08.017. Epub 2023 Nov 30. Erratum in: J Am Coll Cardiol. 2024 Mar 5;83(9):959. doi: 10.1016/j.jacc.2024.01.020. Erratum in: J Am Coll Cardiol. 2024 Jun 25;83(25):2714. doi: 10.1016/j.jacc.2024.05.033. PMID: 38043043; PMCID: PMC11104284.
- Naidu SS, Baran DA, Jentzer JC, et al. SCAI SHOCK Stage Classification Expert Consensus Update: A Review and Incorporation of Validation Studies: This statement was endorsed by the American College of Cardiology (ACC), American College of Emergency Physicians (ACEP), American Heart Association (AHA), European Society of Cardiology (ESC) Association for Acute Cardiovascular Care (ACVC), International Society for Heart and Lung Transplantation (ISHLT), Society of Critical Care Medicine (SCCM), and Society of Thoracic Surgeons (STS) in December 2021. J Am Coll Cardiol. 2022 Mar 8;79(9):933-946. doi: 10.1016/j.jacc.2022.01.018. Epub 2022 Jan 31. PMID: 35115207.
- Ruben M, Molinas MS, Paladini H, et al. Emerging concepts in heart failure management and treatment: focus on point-of-care ultrasound in cardiogenic shock. Drugs in context. 2023 Jan 4;12:1–13.
- De Backer D, Biston P, Devriendt J, et al. Comparison of dopamine and norepinephrine in the treatment of shock. New England Journal of Medicine. 2010 Mar 4;362(9):779-89.
- Jeon Y, Ryu JH, Lim YJ, et al. Comparative hemodynamic effects of vasopressin and norepinephrine after milrinone-induced hypotension in off-pump coronary artery bypass surgical patients. European journal of cardio-thoracic surgery. 2006 Jun 1;29(6):952-6.
- Mathew R, Di Santo P, Jung RG, et al. Milrinone as compared with dobutamine in the treatment of cardiogenic shock. New England Journal of Medicine. 2021 Aug 5;385(6):516-25.
- Gray A, Goodacre S, Newby DE, et al. Noninvasive ventilation in acute cardiogenic pulmonary edema. New England Journal of Medicine. 2008 Jul 10;359(2):142-51.
- Alviar CL, Miller PE, McAreavey D, et al, ACC Critical Care Cardiology Working Group. Positive pressure ventilation in the cardiac intensive care unit. Journal of the American College of Cardiology. 2018 Sep 25;72(13):1532-53